|
Bên cạnh những trường hợp lâm sàng được giới thiệu bởi các Giảng viên của BM, các BS của BV Trường ĐHYD Huế và BVTW Huế, BM Ngoại sẽ đều đặn giới thiệu những case study được đăng tải trên website eMedicine-Medscape trong chương trình đào tạo liên tục (CME) của tổ chức này để bạn đọc tham khảo, tự kiểm tra và đối chiếu với câu trả lời được chọn lựa bởi các đồng nghiệp.
Trường hợp sau đây được giới thiệu bởi Dr Basu S., India

Figure 1.
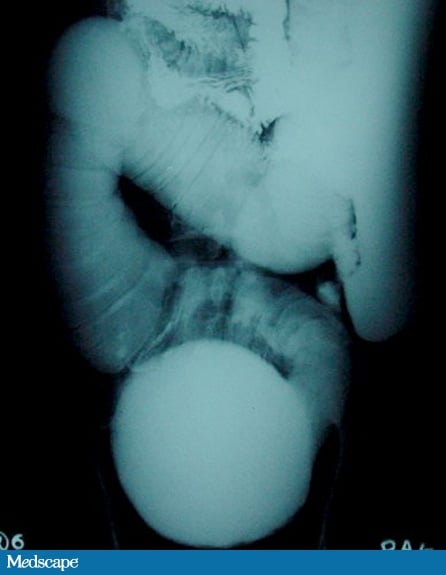
Figure 2.
Background:
A 26-year-old man presents to the emergency department complaining of recurrent, colicky abdominal pain, intermittent distention, and vomiting for the past 5 months. His bowel and bladder habits are normal and he denies any hematemesis, melena, hematochezia, or fevers. He reports no history of tuberculosis, significant medical illnesses, or prior abdominal surgeries. His medications include mefenamic acid and dicyclomine injections for pain, which provide symptomatic relief.
On physical examination, he is a well-developed, pale-appearing man noted to be in moderate distress. His vital signs reveal an oral temperature of 98.4° F (36.9° C), pulse of 98 bpm, blood pressure of 110/70 mm Hg, and respiratory rate of 32 breaths/min. His sclerae are anicteric and his oropharynx is dry. The respiratory and cardiovascular examinations are normal. The extremities are cool and without any cyanosis or edema. The abdomen is distended but soft and nontender, with visible peristalsis in the central abdomen. Swelling is appreciated in the hypogastrium, which becomes prominent during peristaltic waves. He has hyperactive bowel sounds. There is no appreciable organomegaly, fluid wave, or palpable hernia. The genitourinary examination is normal, and the rectal examination reveals normal tone and soft, yellow stool that is negative for occult blood.
The laboratory analysis reveals mild anemia (hemoglobin 9.6 g/dL [96 g/L]), elevated blood urea nitrogen (52 mg/dL [18.6 mmol/L]), and hyponatremia (serum sodium 124 mEq/L [124 mmol/L]). A plain x-ray of the abdomen demonstrates multiple air-fluid levels suggesting a small-bowel obstruction (Figure 1). Abdominal ultrasonography reveals distended small-bowel loops with hyperperistalsis. He is admitted for observation, bowel rest, and intravenous fluid therapy. He is kept NPO (nil per os), a nasogastric tube is inserted to decompress the stomach, intravenous fluid supplementation is started to correct dehydration and sodium loss, and a close watch is kept on his abdominal girth and urinary output. After 10 hours his symptoms are partially relieved and abdominal distention has decreased; however, he continues to experience colicky abdominal pain (although less frequently). Enteroclysis is performed the next day. It reveals dilated ileal loops and pooling of the contrast in a localized, grossly distended segment of the gut in the lower abdomen (Figure 2).
|